Overview of Heel Pain, Heel Spur, Plantar Fasciitis
Heel Pain, Heel Spurs, and Plantar fasciitis are all often described as “A sharp severe pain that hits when first standing from lying down or sitting position. A stone bruise-type pain or burning arches may also accompany this condition.
This pain seems to get better as you warm up or walk it out, but remains a dull ache when standing for long periods. The pain usually returns in the morning or following rest”.
Strain on the plantar fascia is aggravated by over pronation
Pain and inflammation of the plantar fascia and surrounding tissue is an extremely common problem experienced by a wide variety of people. The most common cause of this problem is excessive rolling in of the feet (over pronation).
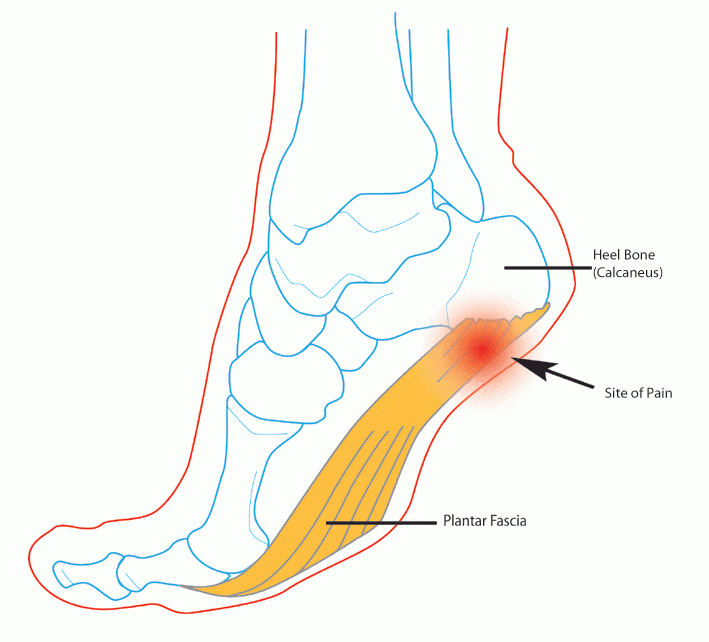
When the feet roll inwards the arch collapses and the foot elongates. This elongation stretches all of the structures on the bottom of the foot (ligament, muscles and nerve) and Achilles tendon causing heel and arch pain where they insert into the heel bone (calcaneus).
The plantar fascia is the main ligament on the underside of the foot. It runs from the calcaneus (heel bone) to just behind the toes. The plantar fascia helps to keep the foot from spreading out and rolling in.
When the foot is not properly aligned the bones of the foot unlock causing the foot to roll in. This places excess stretching stress on the plantar fascia. The plantar fascia alone is unable to maintain the arch contour and with overuse becomes painful and inflamed.
With every step, during physical activity, the foot pronates and elongates. This stretches the plantar fascia and causes heel pain.
Our orthotic innersoles (foot supports) align the foot in the most efficient functional position and maintain the arches of the foot. This relieves the strain on the plantar fascia and reduces foot pain.
Docpods orthotics and footwear come in a variety of styles to suit almost any shoe and offer pain relief.
What is the cause of heel pain?
Plantar fasciitis is the most common cause of chronic heel pain in adults. It has been described with various graphic terms associated with physical activities e.g. tennis heel, joggers heel or policeman’s heel.
Other causes of heel pain
There are other health conditions that cause heel pain. Severs disease, retrocalcaneal bursitis, tarsal tunnel syndrome, stress fracture, fat pad contusion (fatty tissue under the he heel. calcaneal bursitis, bone spurs, stress fractures, Achilles tendinitis, and sever’s disease (growth plate irritation in the heel in children) to name a few.
These are aggravated by foot mechanics, and some are growth-related such as Sever’s disease. We discuss these in our other heel pain articles.
What happens to the foot with heel pain, heel spurs and plantar fasciitis?
Within the foot, there is a tough sheath of tendons that maintains the normal arch of the foot from underneath known as the plantar fascia. The plantar fascia normally has a narrow end that is attached below the calcaneus (heel bone).
The wider end fans out to be attached to the underside of the toe bones. When intact, it maintains the arch of the foot and also acts as a shock absorber for the foot.
This fascia acts like a hammock, bearing the weight of the foot. The fascia normally has elastic and flexible properties that permit free movement of the foot and allow it to perform its shock-absorbing function.
Repeated strain causes injury and pain
Plantar fasciitis occurs when there are repeated small injuries to the fascia, this is usually due to physical exercise, over pronation or poor footwear. These injuries are too tiny to be repaired and occur as a part of daily stress and strain on the foot.
When there are repeated injuries to the fascia, a new tougher scar tissue forms. The new tissue that is formed is often not as supple or elastic as the original one.
This scar tissue gives rise to the condition where the ability of the fascia to maintain the arch is slowly lost, as the plantar fascia is not as flexible as it needs to be.
When the plantar fascia is damaged and becomes scarred, it effectively shortens due to the scarring from injury. When the plantar fascia cools down when at arrest the length of the plantar fascia is further shortened.
This occurs when the foot is not bearing weight when at rest, as happens at night when the person is in bed. As soon as the first steps are taken in the morning, the foot needs to bear weight.
This causes the arch of the foot to flex and the fascia to stretch to bear the weight, like a hammock. It is this stretching that leads to pain, as the plantar fascia is stressed.
The pull at the heel bone, where it is attached, can eventually give rise to the formation of small bone extensions at the heel bone, where the fascia is attached. These are called heel spurs and these aggravate the condition. After bearing weight or walking, the fascia warms up and becomes more flexible.
This relieves the stabbing heel pain however this is only temporary. The inflammation from repetitive small injuries within the plantar fascia remains and the pain also persists as a dull ache.
At the end of the day, the pain regains its earlier intensity, although it is not a stabbing pain.
Cause of heel pain and plantar fasciitis
Repeated stress and strain on the fascia is the common reason for the development of this condition. Over-pronation is the number 1 cause of excessive strain on the plantar fascia.
Excessive weight or obesity is also a common cause, this results in the extra load being placed on the foot and this causes further overpronation. People who need to stand for long hours are also common victims.
Walking or standing barefoot or on hard ground or wearing shoes with hard heels can also lead to this condition or aggravate an existing one. Aging that leads to loss of the flexibility of the fascia is also commonly associated with plantar fasciitis.
Most patients are between 40 and 70 years of age. People with problems in the arch of the foot, like those with flat feet or very high arch, are susceptible to plantar fasciitis. Sportspeople or people who are active can suffer from plantar fasciitis if they have faulty foot mechanics that can result in over-pronation.